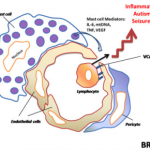
What do chronic illnesses such as Autism, Chronic Fatigue Syndrome (CFS), Fibromyalgia Lupus, Chronic Lyme Disease, Interstitial Cystitis, Multiple Sclerosis, and more have in common? Well, these illnesses may have a lot of things in common, and a lot of overlapping symptoms, but many patients symptoms seem to be compatibled with Mast Cell Activation Syndrome or Mast Cell Activation Disorder (MCAS or MCAD).
So what is MCAS/MCAD according to the AAAAI?
MCAS is a condition in which the patient experiences repeated episodes of the symptoms of anaphylaxis – allergic symptoms such as hives, swelling, low blood pressure, difficulty breathing and severe diarrhea. High levels of mast cell mediators are released during those episodes. The episodes respond to treatment with inhibitors or blockers of mast cell mediators. The episodes are called “idiopathic” which means that the mechanism is unknown – that is, not caused by allergic antibody or secondary to other known conditions that activate normal mast cells.
https://www.aaaai.org/conditions-and-treatments/related-conditions/mcas
A list of triggers for MCAS/MCAD according to The Mastocytosis Society
- Heat, cold or sudden temperature changes
- Stress: emotional, physical, including pain, or environmental (i.e., weather changes, pollution, pollen, pet dander, etc.)
- Exercise
- Fatigue
- Food or beverages, including alcohol
- Drugs (opioids, NSAIDs, antibiotics and some local anesthetics) and contrast dyes
- Natural odors, chemical odors, perfumes and scents
- Venoms (bee, wasp, mixed vespids, spiders, fire ants, jelly fish, snakes, biting insects, such as flies, mosquitos and fleas, etc.)
- Infections (viral, bacterial or fungal)
- Mechanical irritation, friction, vibration
- Sun/sunlight
Symptoms and Triggers of Mast Cell Activation
I know for a fact that many have trouble with one, many, or perhaps all of these triggers. From that list, I know alcohol, stress, sunlight, infections, some natural odors, perfume, chemicals, heat, drugs, exercise and cold trigger my symptoms. I know certain indoor environments can be triggers too — possibly from mold/fungus, bad indoor air quality, or a poorly maintained HVAC system.
The Mastocytosis Society had a decent list at symptoms associated with MCAS/MCAD, but let’s look a little more in-depth at symptoms.
Oh TWIST has a pretty good (and long) list. Yes, the list seemingly go on forever, but these are symptoms that many with MCAS/MCAD will experience.
A Relatively Complete List of Associated Symptoms (Oh TWIST)
- Easy flushing red, particularly of the “mantle” (upper chest, neck and face, not always 100%), and especially to stress, heat or triggers (including emotional)
- Hives, especially stress-driven ones, can be large or small and not always all over
- Urticaria Pigmentosa (persistent hives that fade but never disappear), TMEP, Purpura
- Dermatographism – aka “skin writing” where you either turn red easily or even get a hive-like whelt (wheal) with a light skin scratch. (Google it for images.) You may notice red indented sock & underwear “tattoos” where the elastic rests on your skin in winter
- Adult onset or flare-ups of acne
- Sudden onset diarrhea especially alternating with constipation (often called IBS)
- Sudden abdominal bloating and swelling (can look “pregnant” when you’re not)
- Sudden onset of gas and belching
- Sudden onset nausea, trouble swallowing (rule out comorbid HDCT driven neurological drivers of this), early satiety
- Tendency to run cold (but can alternate with sudden hot flashes/sweating bouts or run hot also)
- React easily (are sensitive) to sunlight, vibration, startling, pressure, stress, hot or cold
- Sensitive to alcohol and molds (the penicillin class of anti-biotics, mushrooms)
- Reaction to bee stings and iodine contrast dyes, local & general anesthesias
- Itching of unknown origin, may migrate, often severe
- Tingling or burning sensation anywhere in the mouth or GI tract (BMS)
- GERD
- Tinnitus of all kinds, but especially after eating certain things
- Variable blood pressure (BP), may run quite high or low on average and can swing widely at times. Some have a spike with anaphylactic reactions, followed by later drop.
- Angio-edema (swelling) especially that “migrates”, e.g., shows up in different places (lips, eyes, hands, feet), not always in the same place nor due to being upright (gravity-driven)
- Shortness of breath and asthma like symptoms and outright asthma
- Hair loss/thinning
- A persistent non-productive but wet-sounding cough with no identifiable infectious origin
- Chronic post-nasal drip or rhinitis in the absence of allergies
- Watery eyes, burning eyes (feeling of granularity or sandiness behind eyelids)
- Rashes of unknown origin, adult onset acne or acne-like spots (not same as Urticaria Pigmentosa which is a form of cutaneous mastocytosis)
- Easy nose-bleeds (epistaxis) of unknown origin, easy bruising or bleeding (w or w/o a comorbid connective tissue disorder)
- Slow wound healing
- Aquagenic urticaria (your skin reacts to immersion in water)
- Sudden weight gain or loss in absence of clear driver/cause (rule out lipedema and endocrine disorders)
- Sudden mood swings, anger bouts or irritability (we call this the “histameanies” in support circles, smile, and thank everyone for tolerating us through them)
- Cry easily, easily aroused, emotional (look into histadelia)
- Sudden anxiety or panic attacks followed or accompanied by additional signs of low-level anaphylaxis (skin signs, mucus, etc.)
- Sudden onset aphasia, or loss of words or speech, slurred speech or “word salad” that clear up after the reaction/stress subsides or with anti-histamines or mc stabilizers (be sure to rule out stroke! as well as epilepsy).
- Any and all forms and levels of anaphylaxis which comes in grades. Many are in mild constant low level state with occasional spikes to higher states or rebound events. (Most medical personnel refuse to call it anaphylaxis until it’s the higher level/s however be prepared for some differences of opinion here and try to stay calm.)
- Sensitivities or anaphylaxis to any and all drugs, fillers, dyes, additives, preservatives, fluoride, chlorine, etc. We can react to any degree to almost anything, truly. (Yes, crazy making for all.) Sometimes it’s not the active ingredient, but a dye or filler. Or the fact you were upset when you ingested it.
- Esophageal spasms, nutcracker esophagus, especially when stressed
- Chronic fatigue, sometimes severe, often identical in onset/nature to opioid-induced respiratory depression (many find this in reaction to gluten and dairy) often misdiagnosed with Chronic Fatigue Syndrome
- Pre-syncope – or dizziness, light-headedness, feeling about to faint (but you don’t)
- Full syncope – full fainting (less common but also happens)
- Confusion, sudden trouble with word-finding, sudden memory-loss (check for stroke tho too, time is of the essence and you’d rather be safe than sorry!)
- Clotting or alternatively bleeding disorders (either direction) that defy normal hematological diagnosis and workup (and treatment)
- Swollen lymph nodes of unknown origin, not true lymphomas
- Any other forms of hematologic disorders (strange cell counts/sizes, changes in same) that do not strictly match true workup for similar conditions (e.g. polycythemia in absence of the JAK2 mutation) or don’t respond appropriately to treatment for same
- Migraines and cluster headaches, hydrocephalus and “corking” driven dysautonomia
- Low blood volume from 3rd spacing and urinating more than ingesting during reactions (lends to BP drops and very low BP)
- Kounis Syndrome or signs of it. (Allergy-type driven MI/vessel spasms)
- Interstitial Cystitis (IC) or chronic UTI’s that don’t resolve easily or at all with anti-biotics (i.e. “sterile” inflammation)
- Women may notice “flares” of these symptoms on a monthly basis from their cycles, and or during lifetime hormonal changes, especially any time after age 30 from peri-menopause
Hypotension (low blood pressure) is common with MCAS/MCAD, but some patients may present with hypertension. Hyperadrenergic POTS can present in Mast Cell Activation Disorders. Hyperadrenergic POTS presents with orthostatic intolerance associated with an elevated heart rate (≥30 bpm within 5 minutes of standing) and hypertension (≥20 mm Hg increase in systolic blood pressure upon standing).
See Hyperadrenergic Postural Tachycardia Syndrome in Mast Cell Activation Disorders in the journal Hypertension.
Is There Research Connecting MCAS/MCAD to Chronic Illness?
Ok, by now, you may be thinking, wow, I have many of the triggers and symptoms on this list, but is there research showing that this condition exists in various chronic illnesses? Dr. Theoharides, the Director of the Molecular Immunopharmacology & Drug Discovery Laboratory, has put out quite a lot of research.
You can check out his huge amount of research here: http://www.mastcellmaster.com/publications.php
Treating Mast Cell Activation
While a lot of Dr. Theoharide’s research focuses on natural substances such as Luteolin for inhibiting mast-cell activation, and while he is the medical director of Algonot, it’s important to note that he receives no compensation from this company. I think it is important to note this fact because often when one has financial ties to companies or products, their research often becomes skewed or misleading. Algonot develops a supplement for MCAD called Neuroprotek that contains the bioflavonoids Luteolin, Quercetin, and Rutin.
There are pharmaceuticals for MCAD. Hydroxyzine preparations can be quite powerful, but usually require a prescription. Anecdotally, the combination of Zantac and Zyrtec (OTC at your local pharmacy) seems to work pretty well. Zyrtec is an H1 receptor inverse agonist and Zantac is a H2-receptor antagonist. However, even though these are over the counter, do not begin these medications without consulting with a qualified healthcare practitioner first.
Is MCAS/MCAD connected to methylation?
This may be the million dollar question. There is not much information and MCAD and methylation, but I will end with a quote from the theory at mthfrheds.com.
MTHFR Polymorphism may be a predisposing factor to mast cell disease. 5-MTHF regulates biosynthesis of BH4. The A1298 mutation in the MTHFR enzyme effects the conversion of BH2 to BH4. Less amounts of BH4 inhibits NO formation resulting in increased mast cell degranulation. Inadequate BH4 formation also puts a strain on the conversion of tryptophan to serotonin and tyrosine to dopamine, leading to low levels of the neurotransmitters: dopamine, norepinephrine, serotonin and melatonin.
Low blood serotonin levels help define a sub-group of patients with mastocytosis that are more likely to present with neurological and gastrointestinal complaints. Human mast cells can express and be activated through multiple serotonin receptors, and synthesize and release serotonin. Low blood serotonin levels in such patients may be the result of low BH4 levels due to 5-MTHF deficiency, the result of long-term malabsorption from chronic inflammation of the gastrointestinal tract or both, as is the case with me.
BH4 is a critical factor in cellular activities such as cell proliferation, cell cycle regulation and differentiation. Could BH4 deficiency secondary to MTHFR polymorphism be one of the fundamental mechanisms that underlie mast cell proliferation?
So the question I am left with is what substances should we try, or how do we modify our methylation protocol when it seems that MCAS/MCAD may play a large role in the clinical picture. In the absence of improvement of MCAS/MCAD type symptoms (without taking antihistamines or Luteolin-based supplements), would taking BH4 directly help? Is BH4 deficiency really the issue?
If anyone has any comments on how to address MCAS/MCAD with methylation supplements, or if they have tried taking BH4 directly, please comment.
I have a genetic BH4 shortage, several Ehlers-Danlos syndrome pathologic genes. I’ve not been tested for the primary KIT gene, kit d816v, but the parts of Kit tested, one is suspect for mastocytosis. I’ve almost died of anaphylaxis a few times, once I coded and had a NDE. I’ve lived on the edge for 62 years and doctors used to make fun of me in their “fatherly” ways when I was young, saying I’m a big baby over an allergic reaction. Now, I just want to feel better. I’ve also lost all my teeth though I’ve done everything I can to save them. I read yesterday that is something else that can happen with long-term mast cell disease. My cortisol level is always low normal to WAY low. My blood pressure runs up and down and a former doctor wanted to know what drugs I was abusing to cause that. I’m exhausted today. I hate doctors. All I saw were white male docs when younger. I’ll never forget the abuse I took from them.
cleo, I have Ehlers-Danlos and one thing i have learned is that Postural Orthostatic Tachycardia Syndrome (POTS) seems to go along with EDS. My cortisol levels are like yours and my heart can be all over the place…If you don’t know about POTS please look into it. I am on meds to help and it’s making a very BIG positive difference for me. Be well and never give up.
If you haven’t already, visit http://www.rccxandillness.com
RCCX Gene Theory
I’ve just commented on this thread to someone else but wanted to make sure you read about RCCX Gene Theory. http://www.rccxandillness.com
I strongly feel this applies to you and will help make sense of things.
MCAD is not the same thing as mastocytosis (as another comment said, mastocytosis is one type of MCAD), so giving the Mayo Clinic definition for mastocytosis as the definition of MCAD is misleading. Some people with MCAD have a “normal” number of mast cells but they react differently than normal mast cells do, releasing excessive amounts of chemical mediators.
Fixed. Thank you.
To improve BH-4 production, ELIMINATE all synthetic forms of folic acid to your diet and supplement with active Folate. Do not take capsules that have dyes or fillers. Try and find very pure forms of your supplements and start slow. This is what helped my family.
Also I don’t know if this will help, but organic yucca helpreduce inflammation in the gut, as well.as reducing ammonia. (MUST be organic bc yucca often grown in soil w lead, cadnium and otjer heavy meta contamination.
Be sure to get nutitional GI workup to test for gut inflammation, mycotoxins, and be sure to test for heavy metals., as all this mames kt worse. If toxic w heavy metalsthose w cbs or suox sulfur defects who cannot tolerate thiols cannot tolerate chelators, but CAN use binders, such as Zeolite Pure (OTC) and prescription Cholestyramine
Good artcile. Glad to see BH4 being emphasized. One big problem is the complexity and all the comorbidiities. Problem I’m having is that I also have all the genetic markers for low DAO, and the meds listed wipe out DAO. So histami e is then worsened.
Also, in addition to methylation defects, I also have both major sulfur defects ( cbs and suox.) So I cannkt tolerate any methylation support, as well as many supplements such as bromelain, for bh4 a d DAO production. , and much is contraindicated. Trying to get BH4. I know that helps (also have defects r/t that) and cant get it for a while now, everyone has been out. So meanwhile prednisone.
Hi, I take Bh4. I took it as a prescription until the FDA regulated it out of availability. Now I take pteridin-4, by Ecological Formulas. Not reimbursed by insurance, but a Bh4 source. I became histemically overactive over the last 2 years from retalliatory spraying with OPs (insecticides and roundup). I have 18 methylation errors. I do sub-q mB12. I also eat a low histamine diet, and other than the vicious neighbor, live chemical free/ organic. If I avoid the toxins, and do my protocols I do well. I tried quercetin, but due to the pesticide damage, I have achalasia. Can’t swallow pills or solids. So I empty the caps onto yogurt. Quercetin tastes like dumpster banana peels. Ugh! Muellin tincture is much more effective for mast cell over reactions. My Yasko methylation protocol vitamins have too many substances that cause histamine reaction, or block DAO. Redox-24 by Advanced Life Research doesn’t increase my histamine reactions. I keep looking for low histamine work arounds. Good luck on your own search.
My daughter 1 year old just diagnosed with this!
I was diagnosed with Hep B way back in 2013 when I was supposed to donate blood to my nephew. It was normal to do laboratory check on my blood hence it was found out that I’m reactive to the illness. I’m very depressed and demoralized since this disease has been unacceptable just like the unpopularity of AIDS. I was so nervous that I’ve got ashamed to talk with other people onward, so my mom subjected me to series of tests so that damage to the liver may be traced. The doctor told me that; YES i am chronic carrier, i was so depressed was thinking of committing suicide, till i came across a forum on internet, about MED LAB TEC who cured various diseases like Hepatitis B, Herpes, liver fluke HIV and others, without wasting time, i contacted them and i get medication from them and after the days given to me, I just went back to my doctor and they also carry out the test again, and i was negative of Hepatitis B. Please contact this MED LAB TEC if you are hepatitis B positive or any kind of diseases herbal medicine are indeed best remendy; their email is: medlabtec(AT)mail(DOT)com
Could a tick borne disease trigger Mast Cell Activation? Several months after an embedded tick bite, I started feeling ill (no fever) and having digestive problems and then after eating beef had food poisoning reactions several times. Trytase levels elevated but no actual allergy showed. I now carry an epi pen. I would like to be tested for a mutation which my Naturopath recommended but don’t know where to get that done and also wanted to be tested for all the tick borne illness but PCP referred me to an infection disease doctor who said they are not experts in tick dieases. I was tested for the 3 most common and they were negative. HELP!
I am a 24 year old woman who has spent her entire life with some unknown illness. No allergist has seen a case of environmental allergies as severe as mine and asthma that responds so poorly to medication. All of the symptoms listed are exactly what my daily life is like. I’ve gone into anaphylaxis 10+ times but we never knew what caused any of the episodes and it’s gotten to the point I just stopped seeing doctor’s besides to get refills for my medication because I’ve lost hope of ever finding relief. I also, have Von Willebrand’s Disease that complicates getting treatment and testing because most doctors are afraid to touch me. How do I find a proper doctor so I can get answers? My 16 month old son has the same marbled, temperature sensitive, uncontrollably itchy skin as me and I know he has whatever I have and I’m terrified of him having to go through the medical hell that I’ve gone through. Any answers would be greatly appreciated. I’m so desperate but I’m starting to lose hope in finding a doctor that will be able to help me.
I see this is an old post and I happened to be scrolling through comments. Have you heard of Xolair (omalizumab)? It has been truly life changing for my son who has been on it for 2.5 years. He has chronic idiopathic urticaria, severe allergic asthma, anaphylactic food allergies etc. It’s a monthly injection through allergy. I’ve spoken to other adults with symptoms like you described. Just thought I would share in case you are still struggling. We have been there ❤️
Oh my! It sounds like you’ve had the same life I have. I gave up hope until this weekend. Going to try again. I have von Willebrand’s Disease also. I forgot about that one. I hope you found a doctor and a diagnosis and good treatment. It is a medical hell. I hope your son has found help.
My doctor has just started my on Alegra once a day to see if that does anything. I have Lyme Disease with extremely high inflammation. Along with most of the symptoms you mentioned above in this article. Hoping that the Alegra can help some. We shall see
My daughter is struggling right now, She had hellp syndrome 2 years ago and her health has drastically gone down since then, She was diagnosed with MTHFR gene mutation- the rarest one and thrombophilia which is a blood clotting disorder. Over the last 5 months she has become allergic to just about everything. She has been in a constant state of a blistery rash on her skin and she has other symptoms as well as heart palps , extreme anxiety, shortness of breathe etc. Now some of the allergies are affecting her face and lips. She went for a very thorough allergy testing that showed nickel allergy and allergies to other chemicals that are in just about all the products used on a daily basis. We are thinking this could be MCAS. What kind of doctor do you see for this? Where do begin? The allergist was basically – this is your life avoid these things…..
For the record, MCAD = the UMBRELLA term for ALL forms of Mast Cell Activation Disease (or Disorders, your choice, but they settled on Disease last I checked) AND… includes MC leukemia, all forms of mastocytosis (including SM) and MCAS, which is the newly recognized diagnosis of Mast Cell Activation SYNDROME. (Masto = too many mast cells in clumps and/or misshapen ones which may also be over active, MCAS = just over active ones that leave you symptomatic much like masto, but in absence of any signs of excess numbers in clumps, deformed/spindle-shaped ones, or the C-Kit D816V mutation found in 80% of SM patients yet.)
Most are using MCAD to mean MCAS, incorrectly. Although truly in the end the activation is the main complaint in all cases usually, so it sort of doesn’t matter. But if you’re going to correct people, please get it right, thanks. Mastocytosis is NOT the umbrella term. Never was. It was just the better known form of the MC diseases for many years. See http://tmsforacure.org for more.
As well as: http://www.wjgnet.com/2218-6204/abstract/v3/i1/1.htm
(A concise, practical guide to diagnostic assessment for mast cell activation disease 2014 Afrin, Molderings in case link doesn’t work above.)
Also, if MTHFR caused hEDS, over 40% of the population would have hEDS. Even I don’t think that’s true, though I’ll buy up to 10% possibly from personal observation. I DO think it’s a contributing factor to our overall illness load, and to MC activation – which may lend to bendiness, we don’t know yet. Treating it will defo help. But basic math alone says it can’t be the main cause. Just an amplifier. I know hEDS patients who are negative for it too. (Yes, they are rare.)
Cheers, Jan in Portland, OR
To me this is a fascinating subject.i see a lot of patients with ehlers danlos syndrome,living in a place, recife, brazil,whre most of the people has ehlers danlos syndrome, a lot of pots and i think i may find a lot of mast cell activation syndrome which i ve just started recognizing. This text is very substantial and i could recognize many of my patients. Many thanks.
Hello. I am 1/8 native Brazilian and Portuguese. Do any of the patients you mention here also have temporal lobe epilepsy, or partial seizures? I’ve had this as long as I’ve had the other. I’ve always put them together as the same thing going on. My bouncing blood pressure has been ascribed to three seizures.
I suffered from severe depression for 20 years and about 90% of the health issues associated with Mastocytosis. My family doctor became belittling and dismissed me as a hypochondriac. I started getting severe hives from head to toe that kept me from sleeping for days at a time.His diagnosis was dry skin…I finally lost it and insisted on getting a referral to an Allergist. I lucked out and ended up seeing an Allergist/Immunologist who had studied at Boston.He almost immediately suspected Mastocytosis, did the tests and it came back positive.
I feel blessed to find this site since I’m becoming allergic to some of my antihistamines (I really didn’t think that was possible).Anyway, Thank You for this site,at least I have some leads that might help me out.
My contribution- For my debilitating Depression the only medication I found that worked for ME was Selegiline which is a MAOI.This class of drugs has been mentioned as being beneficial to people with our condition.Its an old time medicine that many doctors are unfamiliar with and now is used mostly for the treatment of Parkinson’s Disease.However my Doctor (Psychiatrist) only prescribed it as a last ditch attempt.It didn’t benefit me with any other Mastocytosis symptoms.It has a long list of dietary restrictions. ,it interacts negatively with many medications including some antihistamines and decongestants, but at least I now have the will to live and keep fighting.
This article has a fundamental problem. It starts out asking what is MCAD and then gives a definition of mastocytosis. The two are very different, and defining one by the other is incorrect and highly misleading.
The article needs to be rewritten, beginning with the correct definition.
Hello! I’ve been struggling with breathing problems for almost two years – this started at age 23. I used to be a half-marathon runner and exercise freak, but one day while exercising, I feel short of breath and that my lungs were seizing up. It was very scary, especially the first time. I’ve been to SO many doctors (asthma doctors included) and have been diagnosed with 100 different things. One told me I had asthma but I didn’t respond to albuterol. Another told me I had costrochondritis, and I tried anti-inflammatory meds for that which just left me feeling like the room was spinning. I’ve had an echocardiogram, two EKGs, two chest X-rays, and routine blood work. The only things that were off were my blood calcium levels (they were high) and I also had high RBC. I have MTHFR but my doctor said that my homocysteine level was fine, so the MTHFR shouldn’t be causing any of my problems. I’m feeling so stuck and hopeless at this point. I want to breathe freely and fully again all the time and not worry about the next time my chest will tighten. It has completely taken over my day to day life. I no longer am able to exercise, and I have trouble breathing after every single time I eat, too – no matter what the food. I’ve never had to think about breathing before this happened to me two years ago, and I want to be that way again. It’s suspected that I’ve been exposed to toxic mold because I was working in a water damaged building. I got so sick that I had to quit my job (I was developing other symptoms, too, such as low blood pressure, heart racing, weakness, dizziness, horrible rage, etc. I’m now living with my mother in Los Angeles, CA. I’d like to see a mast cell doctor, does anyone have any recommendations? I would also greatly appreciate any advice/help! Thank you so much!
After many years ~~~ We finally found genetic disorder in family ~ son … A1298C … fffinallyyyyyyyy was diagnosed at age 52….~~ Our big problem is getting BH 4 ~~~ & where do U get it now in US.. Also was pulled off market a year ago so we are able to get it thru China till we find local source…. This MTHFR is a hugh complicated disorder ~~ Thanks for all sharing. ~~ Let’s get the Help out nuero Science Dr help’s us
Hi All,
I have Celiac Disease and some form of MCAD with preservatives and high histamine foods as my main triggers. I have gotten the mast cells under control for the most part but suffer still with depression and anxiety. Can you help me with what supplements I should be taking? So far I seem to feel a bit better with a magnesium complex supplement. I did not tolerate well a B complex supplement. I’d appreciate any guidance on this if anyone has had good luck healing from anxiety/depression associated with this illness.
I have been reading this website and all the wonderful member contributions.
Can members please help re my 17 year old son with a chronic mycoplasma infection. He has high IgE with a mast cell activation disorder, immune system dysfunction with low IgM, natural killer cell activity . Also his ammonia levels have been high recently. Is there any connection between mast cell activation and high blood ammonia levels? He has minor liver dysfunction with elevated ALT . What can be done to get the ammonia levels down? Many thanks
Alpha keto glutarate is so helpful
My daughter also has the A1298 mutation in the MTHFR enzyme. She is taking methylfolate for that – a pill size lozenge.
To Charleah in Raleigh.
Dr. Nicole Gill at Carolina Headache Clinic (by Southpoint) is great. She is a neurologist who thinks outside the box. She diagnosed MCAD in my daughter, who has been suffering with migraines since the age of 10 (now chronic) and chronic headaches before that since 7 or 8.
None of the standard treatments for migraine ever worked, and many of them hurt my daughter (topomax, triptans, DHE IV, countless preventatives that all failed) and other treatments we tried didn’t help either (chiropractors, biofeedback, etc).
My daughter is still suffering from chronic migraine and insomnia, but many of the other weird symptoms she was experiencing (flushing) calmed down with Claritin. The standard zyrtec/zantac didn’t work for her, in fact Zantac caused huge stomach pain.
I have to agree with an earlier commenter.
Mastocytosis and MCAD/MCAS are two different things. The former is an abnormal number of mast cells and the latter is a normal number of mast cells but they are highly reactive.
So it’s a bit odd when the original writer of this article describes MCAD by quoting from sources that specifically define mastocytosis.
One link between mast cells and methylation is that one of the primary products of methylation is SAM-e and that plus HNMT (Histamine-n-Methyl-Transferase) breaks down histamine. So reduced methylation could mean reduced SAM-e, which in turn means less histamine broken down and more running around in our bodies.
I also happen to have a SNP related to HNMT, which I have been trying to research. Could definitely be some good genetic data related to all of this.
This is awesome people! Thanks so much for everyone’s contribution! I want to add this to the BH4 topic:
The CBS (cystathionine beta synthase) gene catalyzes the first step of the transsulfuration pathway, from homocysteine to cystathionine. CBS defects are actually an upregulation of the CBS enzyme. This means the enzyme works too fast. In these patients, it’s common to see low levels of cystathionine and homocysteine since there is a rapid conversion to taurine. This leads to high levels of taurine and ammonia. The CBS upregulation has been clinically observed to result in sulfur intolerance in some patients. It has also been observed that BH4 can also become depleted with a CBS upregulation. BH4 helps regulate neurotransmitters and mood. Other mutations, such as MTHFR A1298C, Chronic bacterial infections, and aluminum can also lead to low BH4 levels. Lack of BH4 can lead to mast cell degranulation and possibly mast cell activation disorder (MCAD).
MTHFR A1298C is involved in converting 5-methylfolate (5MTHF) to tetrahydrofolate (THF). Unlike MTHFR C677T, the A1298C mutation does not lead to elevated homocysteine levels. This reaction helps generate BH4. BH4 is important for the detoxification of ammonia. The gene is compromised about 70% in MTHFR A1298C (+/+) individuals, and about 30% in people with a heterozygous (+/-) mutation.
BH4 acts as a rate limiting factor for the production of neurotransmitters and catecholamines including serotonin, melatonin, dopamine, norepinephrine, and epinephrine. A MTHFR A1298C + status may cause a decrease in any of these neurotransmitters or catecholamines. BH4 is also a cofactor in the production of nitric oxide. A dysfunctional BH4 enzyme may lead to mental/emotional and/or physical symptoms. Mercury, lead, and aluminum may act as a drain on BH4.
I’d be grateful to know anything more people find on BH4 (biopterin). Like, does anybody know if there is a relationship between BH4 and bupropion?
Resource: Dr. Ben Lynch is doing a lot of good research and teaching (but no consultations right now). See mthfr.net and seekinghealth.com and seekinghealth.org
https://www.novapublishers.com/catalog/product_info.php?products_id=39948
Chapter 6 by Dr Afrin is free to download.
I was diagnosed with mcad after visiting dr after dr. Now my wbc is at 14,000 which has come along way from 31,000. Now I struggle with Major depression disorder and generalized anxiety disorder that followed the mcad diagnoses. My question is, Is this common in people who also suffer from mcad? I am tired of psychiatrists changing my meds, if it is something within the mcad that can be done. I have been doing some research and I have read where serontonin levels have been messed with…..Any suggestions? I go to my Oncologists later this month and my psychiatrist later this month as well, I am at a loss and do not know what to do….
I found this online and wondering if there is any help for patients who have pots syndrome, pelvic congestion syndrome and a rare skin disease called mid dermal elastylosis that is a connective tissue disorder which causes loss of elastin? I have been diagnosed with all of these, amongst others. I am very sick and my health is declining very fast. I have been ill since age 5 and 40 now. I am bedridden at this point and being neglected by drs due to my complexity and the cost and effort it will take to find the underlining mystery illness that has caused all of my conditions and causing me to rapidly worsen. I have every symptom that mast cell activation disorder causes and would make sense to my diagnosed conditions. This is effecting every organ system. My skin, blood vessels, stomach, fainting, allergy symptoms, eyes, kidneys , immune system, tissue under my skin, sinus’s, joints, neuropathy, nervous system, cyclical vomiting syndrome, sensory dysphasia, severe pitting edema, facial flushing and swelling, difficulty breathing, wheezing, severe head pain and fainting after bowel movements, seizures, severe inflammatory response after procedures, a kidney tumor that was inconclusive and set off the underlining condition and many complications that baffled my urologist, a comment from a surgeon when I had a procedure of, ” I’ve never seen such a severe inflammatory response as you in my 35 years in my practice ” and I am terrified for my self. Mast cell activation disorder would make sense for everything but no dr wants me or is willing to try to help me. Because my illnesses and being so sick gives me anxiety, these drs blame my symptoms solely on anxiety and my health is suffering. I am now on disablity and feel that if I had a Dr willing to care, I could get better and work like I love. I would give anything and everything I have to get the care I desperately need and deserve. I have a dr and cco who cares more about their money than their patients. I am in a horrible situation and at this point, to sick, to hopeless and to scared to start over with another dr who will only treat me the same. I have been abandoned by drs because of how complex I am and that hurts. Please help me!! I will do anything!!! My dr is keeping me sick and it’s ruining my health and life. I have so much to offer in this life and want to donate a kidney to a patient needing one. I need to get better in order to help save someone’s life. Please, help me..
Has anyone tried cromolyn sodium orally to treat MCAD or food intolerances? maybe just a short stint on it to reduce inflammation and allow healing?
I use NasalCrom, which has cromolyn sodium in it, and it works miracles! The asthma inhaler type they are discontinuing in the US. Probably to sell us another expensive drug instead. Yes, I find it helps me very much. Five years late, but I hope you’re doing ok.
Konatyme…..Dr Chin in Long Beach Memorial Children’s, Ca. Very well versed in mast cell issues. A lot of us fly to see him. He sees adults too
GREETINGS ………to every body , i am MORRISON BELL from LONDON(UK). I was once diagnosed with LUPUS in September 2014. I back than i was having skin rashes all over my body, this was very unbearable to me , then life was without meaning to me due to my health status , i tried my possible best to get cured but all seems in vain, So all through those period of my life, i was unhappy.
I still kept doing research on possible cure for LUPUS since 2014 though i knew science has no cure for it yet, few years ago while i was on search in the Internet i came across different testimonies on how this great man called DR.ODIGIE has been saving souls with his herbal medicine , people recommended that he has been using his medicine to cure LUPUS and different disease permanently and they advice that anyone who haven’t get in contact with him should contact him now for help.
So After reading several testimony from different people concerning DR.ODIGIE medicine for curing LUPUS , i said to myself that God could use any means to heal his servant , So without any doubt, i contacted him about my LUPUS Diagnosis treatment ,i explained my problems to him, without wasting time, he told me that he is going to help me , So he prepared a herbal medicine for me which he sent to me and he told me to use it according to the instruction that i will see on it, so i abide to him, before i know it, i was beginning to feel some changes in my body , the skin rashes i had on my body was gone and so i went for medical check up and to my greatest surprise, i was healed and cured from the disease i tut then can never be cured from my LUPUS but DR.ODIGIE gave me reasons to live , I am so very happy now as i am sharing my testimony and i want to use this medium opportunity to tell anyone who is having this sickness LUPUS or any kind of disease like HERPES, HEPATITIS B ,DERMATOMYOSITIS .HIV AIDS, Cancer, syphilis, gall stone and lot’s more should quickly contact DR ODIGIE on his email at:(drodigiesolutiontemple at yahoo.com) . His Herbal medicine is one of a kind and i believe he can also cure you too just as he has cured me..THANKS
you can go to facebook mast board. and many others as an additional info with people having this.
Carol,
thank u. I am in Southern California, can I google a certain type of Dr to find 1 out here? Is there anything I can do right now to start treating? Has anyone one tried Cromolyn sodium?
thanks
Konatyme,
Feel for you. Dr. Marianna Castells, and Atkins are great at BWH in Boston.
my stomach biopsy shows 14-16 Mast cells per high definition slide. also multiple eosinophil cells floating around my gut. I went to UCI immunology and they tell me it is not normal to have mast cells in my gut but they can do nothing for me. I am extremely ill. I have 3 small kiddos and I really need some help. What type of Dr do I go to diagnose ( or not diagnose) this and then to get some treatment? many thanks
Drupal is one of these effective software packages that helps people and businesses publish content on their websites.
Figure out what it is you need and want and from there shop around
to see what web hosts matches these expectations.
What search results will offered up with unless you possess a website or perhaps a blog to market your business.
I’m delighted to find all of you and the information you’re sharing. perhaps you have some suggestions for me. i was dx with Mast Cell Activation Syndrome about 10 years ago. The only symptom i had was stomach cramping- gastrochrome, loratidine and famitodine helped and I was essentially symptom free. I was diagnosed also around the same time with a IGG subclass deficiency which explains why for all my life i’ve gotten respiratory infections at the drop of a pin and ones that linger incessantly. Of late I feel everything triggers my mast cells and everything i’ve tried has failed to calm them- low histamine foods don’t make a difference, and I’m at wits end. I ‘m a highly energetic person who’s sick ALL the time now with either an infection or mast cell activation- in part from the infection. Exercise and sun are so troublesome I can only walk- and when i’m well- which is rare. I have two MTHFR variants; 677 C>T and 1298A>C. A PCP advised me to take folate supplements and I’ve taken high potency B tablets. I hadn’t noticed any connection between folate supplements and reduced mast cell activation. I had my whole exome sequenced and found nothing pathogenic. A couple of variants of unknown clinical significance were found- 3 of some attenuated use including though a heterozygous 1366C>T in the SLC46A1 gene- and this variant is associated with hereditary folate malabsorption- which is linked to recurrent infections( i have) and chronic diarrhea (i don’t have) I feel I’ve reached the limits of what medicine can offer and am desperate to feel better and get back to living my life- aka working- at least part time and exercising. Can anyone help with suggestions? Appreciate your thoughts.
HI Barbara,
Dr. Marianna Castells at BWH, Boston is an expert in MCAD and could potentially help you.
Carol
Are you sick? Have you been battling with strange and funny illnesses? Are you in a situation whereby the doctors have done necessary tests and said there isn’t anything wrong with you? … These were all my stories until I met with a total cure for them all… His name is Dr. Payo Shalo says my mom… I was almost at the point of death. It was that serious that I was just placed on life support even as the doctors didn’t know what was wrong with me. My mom just came to my hospital bed one morning and said she had found a solution to all of my sufferings (because that was what I referred to the situation I was in then)… She said she was going through the internet and she came across some testimonies of how some people who had similar cases as mine were all cured off their illnesses through the power of this voodoo man. Without hesitation, I told her to contact the man, Which she did and she went on with the procedures as instructed her by this voodoo man (these procedures, I wasn’t aware of because I was in a really bad shape then, And whenever I asked my mom she would say I shouldn’t bother myself about that…that it was something she could handle). Not to bore you readers with too much of my story, in seven days from that day my mom told me about the voodoo man, I was cured off this killer disease that was at the verge of taking my life. Want to share your testimony like me? Contact the voodoo man on his direct email address… payospiritsshalospells’’AT’’yahoo’’DOT’’com (rewrite the email in its right form)… I AM NOW A HAPPY AND HEALTHY YOUNG MAN ONCE AGAIN…THANKS TO DR. PAYO SHALO
Hi Barbara,
I have some ideas that could help from my own experience and research. Feel free to contact me directly at RootBasics@gmail.com.
Judy
Chronic inflammation from Biotin Illness, such as Lyme, genetic mold illness (chronic inflammatory response syndrome see survivingmold.com) can often be the initial trigger for MACD. Just learning about all this but believe this is my debilitating issue beyond the Biotin Illnesses I have. My symptoms for the last 15 years has been episodes every 30-32 minutes (consistently without break), 24/7–really!! They start with sudden onset of anxiety-terror, heart racing, air hunger, nausea, intense heat and the profuse sweating, and chills between these episodes. I often feel I am dying with these episodes. I also have symptoms of and diagnosed with Bartonella and other co infections, Fibromyalgia, CFS, IBS, Blapheritis, POTS, and more. I have the majority of symptoms on the MACD list. Anyone ever heard of these episodes connected with this. I have been to about 50 drs since the ’80s, and about 35 since 2000 and not only do they have no idea what could cause this they won’t even discuss it with me. They listen then go on like I never said anything.
Thanks,
Barbara
Thank you so much for this article, and everyone who commented, thank you for the information!
I encourage everyone who sees this to be very cautious (ie, avoid like the plague, but make your own decision because I’m not a doctor and this isn’t medical advice) with fluoroquinolone antibiotics – cipro/ciprofloxacin, levaquin/levofloxacin, avelox/moxifloxacin, floxin/ofloxacin, and a few others. They deplete mitochondrial DNA, induce a massive amount of oxidative stress, deplete antioxidants, and trigger mast cell activation. Of course, this means that they can lead to multisymptom chronic illness in some people. Here are some posts, with links to articles embedded, connecting fluoroquinolone antibiotics to oxidative stress and mast cell activation:
http://floxiehope.com/2013/11/15/antioxidant-depletion-by-fluoroquinolones/
http://floxiehope.com/2014/08/05/cellular-damage-fluoroquinolones/
http://floxiehope.com/2015/10/01/can-fluoroquinolones-activate-mast-cells/
I have these same symptoms but the triggering toxin is exposure to nonionizing radiation. Those who are triggered by this are often left out of this problem. Many get triggered by chemical exposure and then later but nonionizng radiation exposure. Avoiding these exposures keeps the symptoms at bay–however this is increasingly impossible due to the ubiquitous nature of these triggers. Please include wireless radiation and EHS in your studies as we are in desperate need of recognition. Thank you.
Could someone tell me all the test that you need to diagnose this.
I have periperal nerve damage in vesitublar system and some problems associated with MCAD. I would like to get in touch with Sabry Magdy from Egypt as I have GIT involvement and peripheral nerves. Could you please get in touch with me as I am in United States and can direct you to people here. I also would like to discuss your symptoms as they are similar to mine.
E-mail me at mdl09@comcast.net.
Jennifer,
I applied to your Facebook page, It says it is a closed group, I was diagnosed with Fibromyalgia and chronic fatigue 11 years ago, My whole life I have reacted to strangely to things. ,Allergic to mold, dust , heat a lot of smells. But just started putting all the pieces together, strangely after I started eating health high histamine foods, and tinnutis ( does that ever go away). heart rate soring after certain foods or just standing. AND NO SLEEP. That is big. Any ideas on sleep? I got the 23 and me done. I am hetero1298 and 677, homo MAO, hetero DAO and homo BH8,and others. I live in Raleigh NC. Not far from Duke, it seems that this is something brand new when you talk to the doctors. I need a doctor that understands how to test and treat, I am 58 and tired. My son had all of the same mutations, my fight is for him more for me, It would me great to get some answers so he can live a full life.
i am a professor of ENT from Cairo Egypt.
i am one of the victims of MCAD which i suffered from all my life and have just recently beingdirected to go through the diagnostic trck for such lifetime illness.
It affected all my body organs but mostly GIT and spine with lately affection of peripheral sensory nerves.
I hope it can be clearly diagnosed and treated not siming full cure but at least a reasonable tolerable form of living with arrest of further deteriorstion.
Hi Everyone.
I run a Facebook group called Mast Movement that mainly focuses on Mast Cell Activation Syndrome. We have over 70 files, a welcome packet, doctor’s list, and basically how to navigate this disorder. I had a very severe case of POTS and it has been eliminated with effective MCAS treatment. Please feel free to come check out the page!
Having an MAO A & B genetic mutation is not totally unheard of condition, you are basically on a non-selective MAO inhibitor. Get your doctor to understand that and maybe they won’t kill you or vice versa. Mast cell activation and hyperadrenergic POTS are both out of control norepinephrine. Norepinephrine promotes cortisol normally which is an anti-inflammatory however without the enough cortisol to shutdown the norepinephrine will active immune cells and mast cells are the first responders.
Please research high unbound copper (copper toxicity) and it’s relationship to histamine response … Also lithium oratate helps regulate serotonin…. Are you low in lithium??? Check a hair test… $90 direct health care access online…. And discover Walsh institute and mensah medical group and find relief for your methylation and histamine issues!! if you need help discovering if you’re copper toxic please find me on Facebook…. Dana Summers… Best wishes to everyone on the health journey
My 8 yr. old daughter has just had labs come back with high typtase and we will be doing more testing down the line of mcas. Doctor wants us to do “kit asp 816 val mutation analysis”, does anyone know about this testing? All I read about here is the 23 and me?
Thank you all for all your amazing information on this site!!!